The call came on a Tuesday. The call I’d been expecting. The call that would deliver the results of my breast biopsy. I wasn’t worried. Despite the fact that two of my sisters had previously been diagnosed with breast cancer. For some reason, I didn’t feel it was in the cards for me.
“What will you do if the results come back positive?” my husband asked over breakfast the previous Friday, just after the biopsy.
I shrugged. “That’s a no brainer. I’ll tell them to take ‘em both.”
I’d just pulled into the parking lot at work when my doctor called with the results. “No cancer,” she said.
“Great,” I replied, not surprised by the results.
“However, they did find some atypical cells. I’m afraid you have another surgery in your future. A lumpectomy, at a minimum. Unless you choose to have a mastectomy.”
My heart leapt into my throat. “Whoa, wait a minute. Mastectomy? Just what exactly are you saying?”
“You have a condition called Atypical Lobular Hyperplasia…”
ALH is a pre-cancerous condition in the milk lobes of the breast which may, or may not, become cancerous. The more risk factors you have, the greater your chances that it will develop into cancer. My doctor pointed out that with two direct relatives who have had breast cancer, along with several other factors, my odds of getting breast cancer were pretty high.
Suddenly, my mind was a whirl of choices, none of which seemed like the right choice. Still in a daze from the news but determined to gather as much information as possible before I made my decision, I went to see a series of doctors.
The Decision:
The first stop was a breast surgeon. I thought I was going to discuss all of my options, but as it turned out, I was there to discuss a lumpectomy (the removal of the tissue surrounding the affected area—which had been marked with a dot during biopsy).
Pros: A lumpectomy might remove all the affected cells.
Cons: It might not remove all the affected cells, which would require further surgery.
My second visit was to an oncologist, where we discussed the use of Tamoxifen (an oral chemo drug) to stop the spread of the ALH.
Pros: It is a non-surgical (non-invasive) way to treat the condition.
Cons: Tamoxifen has many unwanted side-effects, not the least of which is instant menopause (may be temporary or permanent).
My third stop was to another breast surgeon to discuss preventive mastectomy. Dr. Nima Grissom explained to me that, because ALH is contained within the lobes (or the ducts in the case of atypical ductal hyperplasia) it is difficult to detect because it doesn’t show up on imaging until it has progressed to invasive cancer. Mine was detected because they were testing a suspicious calcification (which was fine) and just happened to capture some atypical cells surrounding it. Which is why doing nothing was not an option for me.
Pros: It would provide a total cure (assuming they didn’t find any actual cancer in the pathology).
Cons: It’s major surgery.
My final stop was to a genetic counselor to discuss my family history and to better quantify my chances of someday getting breast cancer. The genetic counselor took a detailed family history and explained that, even though my sisters both tested negative on the genetic testing, it was very possible that their cancer was in fact genetic, that geneticists can only test the genes that they know today are linked to breast cancer (and that there are very likely many more yet to be discovered).
The bottom line from the genetic counselor: my chances of getting breast cancer at some point in my life were very high, likely greater than 60%.
This begged the question: If I knew that the plane I was boarding had a 60% chance of crashing, would I get on it?
Answer? No. I chose bilateral mastectomy.
What to Expect After Mastectomy:
Mastectomy is not for everyone. One of my sisters chose it, the other did not. It’s a very personal decision that should not be made lightly. Even given my odds, it was not a no-brainer. And even after I made it, I wondered if it was the right one.
What if, I asked myself, the pathology report came back and the only thing they found was that tiny bit of ALH from the original biopsy? It’s not that I wanted them to find something more, but could I justify removing both of my breasts for such a minute amount of pre-cancer?
Answer? Yes, because I did not want to live with the fear of wondering if that tiny little spot would turn into something more. I also knew that there was a distinct possibility that it might’ve already turned into something more.
And so, one year ago today, I underwent a bilateral nipple-sparing mastectomy. A few days later, the pathology revealed extensive amounts of bilateral carcinoma in-situ. Cancer that is contained within the ducts or lobes. That tiny spot had indeed grown into something more.
Things the Doctors Don’t Tell you about Mastectomy:
The Pain:
It hurts. Like hell. But I have a high tolerance for pain and this didn’t bother me. Too much.
The Numbness:
After a mastectomy, you lose all sensation in your breasts. Getting used to the numbness takes time.
The Complications:
My friend Susie Lindau (to read her Boob Report, click here) underwent a bilateral mastectomy five weeks before I did. She sailed through with only one minor complication.
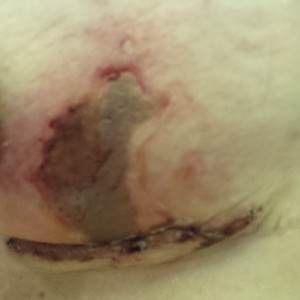
Five weeks after my mastectomy, I had a second surgery to remove a patch of skin that died. The surgery itself was easy (compared to the first one), but because of this condition, I had to take antibiotics for six weeks, which made me pretty sick.
And now, six months after my reconstructive surgery, I’ll have a fourth surgery to remove a capsular contracture.
The Emotional Toll:
This by far has been the hardest part for me. A few weeks after the mastectomy I began crying for no discernable reason. And I couldn’t stop. Medication helped, but for a long time, no matter how hard I tried, I could not summon the joy I used to feel every day of my life. But time heals all. A year later I’m finally beginning to feel like myself again.
Someone asked me recently if, knowing everything I know today, I would still make the same decision.
Answer? Yes. I have no regrets. It’s been a long journey—and it’s not over yet—but I’ve learned a lot about myself this past year. I’ve learned that I am stronger than I thought I was (my surgeon, Dr. Gabriel Kind, calls me “one tough Chicago chick”), and that it’s okay to vulnerable (and to ask for help).
Oh, and because getting pissed off is sometimes the only thing that feels good, I’ve learned to embrace my inner bitch.
Dear Reader,
As an indie writer, we depend on our loyal readers, friends like you, to share our stories and posts. To help spread the word about us.
If you enjoyed today’s post, please share it with your friends using the share buttons below. ↓
If you’d like to know when my next post is up, please subscribe on the sidebar up there to your right.
Thank you for your time and support. I know how precious it is!













L. E. Carmichael
Congrats on your one year anniversary, Suzanne. My mom was a tough chick too – she survived almost 2 years after a diagnosis of 4th stage lung cancer. You never know how strong you are until you have to be.
Hugs.
Suzanne Vince
Wow, Lindsay, I’m so sorry about your mom. How awful it is to watch our loved ones suffer. I was lucky, actually. I didn’t need chemo. It was my biggest fear. I got off easy. *hugs*
Suzanne Lilly
You know, I think “one tough Chicago chick” fits you perfectly! You go, friend!
Suzanne Vince
🙂 Thanks, Suzanne!
Constance Cedras
Suzanne, this is like a primer on everything a patient should do to research and prepare for a major medical decision. I’m so pleased for you that you’ve come through this very difficult year with wisdom and restored health.
Suzanne Vince
Thanks, Connie. That was my intention. I wish I’d found something like this before my mastectomy. It wouldn’t have changed my mind, but it might’ve better prepared me. Thanks for stopping by.
Patricia
Has it been a year already? Wow, I remember the car ride to Tahoe when you were still dealing with the “should I,” or “shouldn’t I” question. It was a tough weekend for you, I remember how much you appreciated having the camaraderie of women to help ease the angst.
I’m so glad everything worked out okay for you and that it was the best decision in the long run.
You’ve got this. You are a mighty warrior.
Patricia Rickrode
w/a Jansen Schmidt
Suzanne Vince
Noble warrior. Okay, mighty too 🙂 Thanks for all of your support this past year, Patricia.
Karen McFarland
Wow Suzanne, what a year. Unless someone has been through something like this, it is impossible to understand everything that you’ve gone through. We just can’t.
I am so grateful that you, Susie Lindau and Christine MacKenzie have spoken out about your personal experience with this dreadful illness. It’s horrible to have your body torn apart. You must be exhausted.
So glad that you’re feeling better. Hang in there and keep on keeping on. You’re an inspiration to us all! 🙂
Suzanne Vince
Aww, thanks Karen!
Cathy McGreevy
So glad you had the courage and wisdom to make the right decision on a very difficult call. It’s good to hear that after a very tough year you are starting to feel like your old self again! Hope it’s nothing but roses from here on out.
Suzanne Vince
Thanks, Cathy 🙂